15-20 internal rotation External rotation stress radiographs for reveal latent diastasis in non-displaced MF Widening of the tibiofibular and/ or medial clear space of >2 mm is considered to be pathological Maisonneuve - like” #s in cases with an intact fibula (so-called “sprains of the tibiofibular joint”), with or without dislocation of the fibular head in the proximal tibiofibular joint.Examination of the stability of the fibular head in the proximal tibio fibular joint may point to an injury to the syndesmosis and the IOM. The tibio fibular squeeze test (compression of the fibula against the tibia), external rotation of foot against the fixed lower leg. Patient present with pain and swelling at the malleolar region.#of the posterior tibial tubercle or rupture of the posterior tibiofibular ligament (PTFL) Rupture of the anteromedial joint capsule or avulsion #of one of its bone insertion #of the proximal part of the fibula Rupture of the deltoid ligament (DL) or a # of the medial malleolus plantar flexion of the ankle in cases of rupture of the anterior talofibular ligament. Rupture of the ATFL or an avulsion #at one of its insertions, with either being associated with rupture of the interosseous tibiofibular ligament.Subcapital #of the fibula associated with rupture of the anterior tibiofibular ligament #of the proximal quarter of fibula, at least, with rupture of the anterior tibiofibular ligament (ATFL) and the interosseous tibiofibular ligament. Anatomic reduction of the distal fibula into theįN is the most important prognostic factor. Under direct vision and intra- or postoperative Open reduction of the tibiofibular syndesmosis MF of the Ankle is ATFL lesion and a highĪssociated #s such as posterior or anterior Reduction of the distal fibula into the Fibular Ankle # with syndesmotic disruption, the most Suture-button syndesmosis fixation: accelerated Thornes B, Shannon F, Guiney AM, Hession P, Masterson E. Suture button fixation is simple, safe, effective,įaster recovery, no need to remove implant. Syndesmosis screw fixation at 3 months, at 12 Prospective, randomized study comparing two methods of syndesmosis fixation. Tricortical versus quadricortical syndesmosis fixation in ankle fractures: a After 1 year no significant differences between the 2 Result was syndesmosis fixation with 2 tricortical Tricortical screws were removed only in the case of Quadricortical screws were removed after 2 months Two 3.5-mm cortical screws engaging only 1 cortex of 4.5-mm cortical screw through both tibial cortices (n = Arthroscopic findings in Maisonneuve fractures. Yoshimura I, Naito M, Kanazawa K, Takeyama A, Ida T. Identifying a/w intra-articular lesions in MFs. During surgery, arthroscopy performed on 4Ĭases mean age 24.5 and result helping in Patients are mobilized with protected weightīearing with a special boot or a cast for 6 to 8 A short leg cast or splint is applied until there Insertion of the 2 implants at 1 to 4 cm above Implant placement >4 cm above the tibial Suture button with 1 or 2 solid screws forĪxially unstable high fibular #s, including MF. Fixation ofAL distal tibia and fibula via a short Displaced PM # PL approach with the patient ORIF MM or DL repair are performed via a AM/PM may also be reduced and fixed via a Bump is placed beneath the calf in order toĪvoid ant. Distal tibia and the ATFL requires short AL For non displaced #s without latent diastasisĢ. interposition of the ligament prevents reduction medial instability following fibular fixation Internal fixation of a proximal fibular #is not ER, displacement, and shortening of the fibula Main goal anatomic reduction of the distal Distal Tibia and the Distal Fibula distance a/w Anterior/posterior/lateral malleolus, lateral Injury to the Tibiofibular Syndesmosis and the Injury to the Proximal Aspect of the Fibula Arthroscopy allows excellent accuracy in the
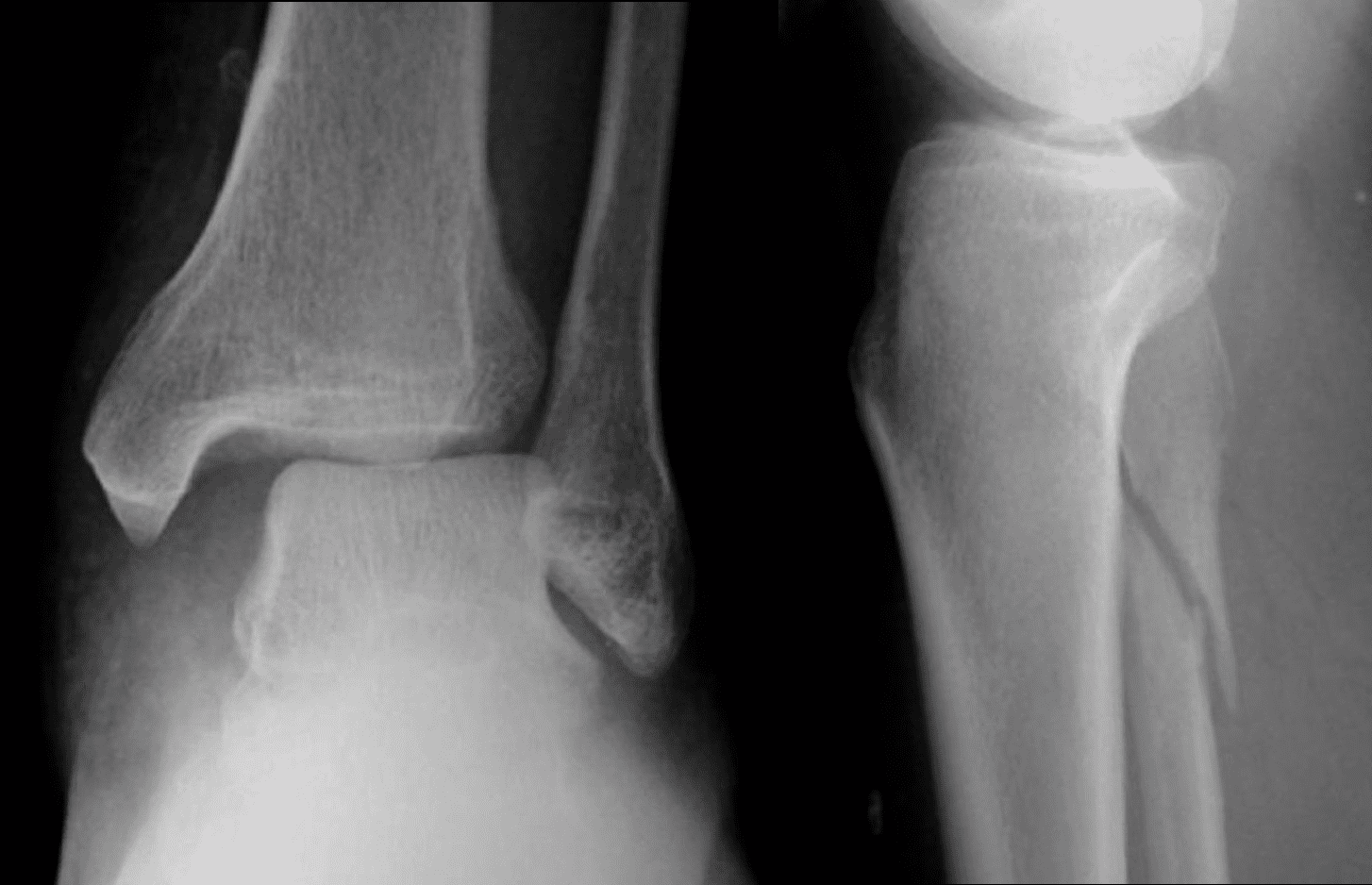
MRI to look for ligament injury but not on Recently advances on weight-bearing in CT 5th and 6th decade for men and women resp. Defination – Fracture of the proximal 1/4th of
